The global and national mpox situation is developing rapidly. Guidance may change as the situation evolves
MPOX VACCINE: UPDATED 20/08/24
Mpox (formerly known as mpox) is a viral infection which is related to smallpox and causes a range of symptoms including lumps or ulcers (sores) on the genitals and/or skin elsewhere.
In 2022, an outbreak of sexually transmitted mpox was identified caused by clade (or strain) 2b. This strain was mainly in gay, bi and other men who have sex with men (GBMSM), in parts of the world where mpox was rare. In the UK, a widespread vaccination programme was undertaken using smallpox vaccines.
In August 2024, the World Health Organisation (WHO) declared a public health emergency of international concern (PHEIC) in relation to the rise of mpox cases. These are linked to clade 1, which have been detected in the Democratic Republic of Congo (DRC) and an increasing number of neighbouring countries. One case has been detected in Europe that was associated with travel to the affected region.
Clade 1 also appears to be transmitted through sexual networks, and is affecting key populations in DRC and surrounding countries. However there is currently no evidence that GBMSM in the UK are at any increased risk of clade 1 mpox. There is on-going transmission of clade 2b mpox amongst GBMSM in the UK, although case numbers are currently much lower than when the outbreak first arose here in 2022.
MPOX VACCINE:
Sexual health clinics in London offer Mpox vaccination to individuals at risk of getting clade 2b mpox via sex. The immunization programme is focused on gay, bi or other men who have sex with men who:
- Have been diagnosed with a sexually transmitted infection in the last year; OR
- Regularly have sex with new partners; OR
- Are taking PrEP currently
You should not have the vaccine if you are:
- Allergic to chicken or eggs
- Allergic to gentamicin or ciprofloxacin antibiotics
- Currently experiencing a high fever or have other possible m-pox symptoms
The vaccine is very safe and most people get no side effects. Some people have temporary mild flu like symptoms such as fever, aches and tiredness. Others may get itching or soreness at the injection site. Two doses at least 28 days apart offer the best protection against mpox, although you are likely to get significant protection after one dose. You do not need a 3rd (booster) dose even if your last dose was some time ago. The vaccine offers protection against both clades 1 and 2.
If you are a gay, bisexual or other man who has sex with men (GBMSM), if you are involved in sex work or if you feel you are at high risk of acquiring mpox through sex, please contact us to discuss the vaccine.
For others in the UK:
- If you are intending to travel to DRC or neighbouring countries, please do NOT contact us about mpox vaccination as we are not authorised to issue travel-related vaccines.
- If you have recently travelled from the DRC or neighbouring countries and you had sex there, or think you may have come into close contact with someone with mpox symptoms, look out for symptoms of mpox (including fever, headaches, and the appearance of a rash or lesions anywhere on the body) and contact NHS 111 for further advice.
SYMPTOMS OF MPOX
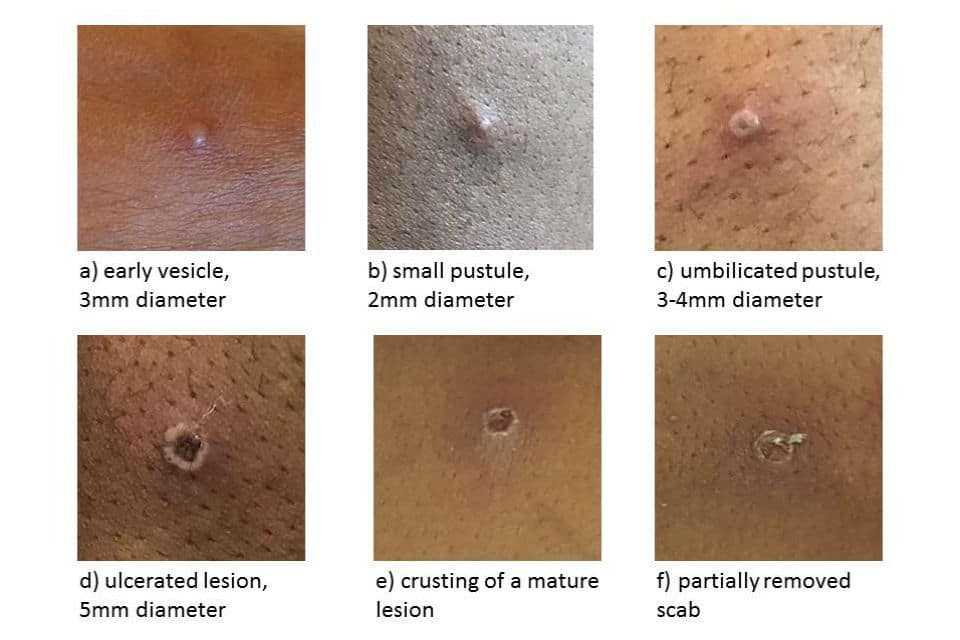
Symptoms begin 5–21 days (average 6–16 days) after being exposed to the virus. The first signs are a high fever, muscle and joint aches, swollen lymph nodes and a severe headache but some people may not have these initial symptoms. Approximately 1–5 days later a rash appears. The rash often starts on the genitals or face before spreading to other parts of the body. The rash changes and goes through different stages before finally forming a scab (see pictures below). Someone with mpox is infectious until the last scab has fallen off.
Clade 2 mpox is usually mild and most people will recover within a few weeks without any treatment. Occasionally, people become more unwell and require hospital admission, so if you have been diagnosed with mpox, let us know if your symptoms worsen. People with clade 1 mpox may require more intensive medical input.
HOW IS MPOX ACQUIRED?
Mpox does not spread easily between people. Person-to-person spread may occur through:
- Direct contact with the skin lesions or scabs.
- Contact with clothing or linens (such as bedding or towels) that have been used by an infected person.
- Breathing in droplets from the coughing or sneezing of someone who has a mpox rash
WHAT DO I DO IF I THINK I HAVE IT?
Call us on 02033155656 for advice if you become unwell with a fever and then develop a rash on your genitals a few days later. Please don’t walk into the clinic. Avoid skin-to-skin contact with others. Don’t share plates, cutlery, bedding, towels and other linen. Avoid sex until you’re given the all clear.
If you test positive, continue to isolate until the last scab comes off. If you have to travel (e.g. a hospital appointment), you should ideally walk, cycle or be driven in your own car. If you have no other choice, wear a mask and cover any lesions on public transport.
Some people are at increased risk of complications for mpox. So particularly avoid contact with these groups
- Pregnant women
- Children under 12
- Immunosuppressed people (HIV positive people not on treatment or with a CD4 count under 200)